
Hospital to home: Automated oxygen solution looks to help patients breathe easier
It takes Lisbet Thobo-Carlsen several hours to get dressed and ready to leave her house. But then, she doesn’t leave her house that often. Diagnosed with severe chronic obstructive pulmonary disorder (COPD) four years ago, she relies on a near-constant supply of supplemental oxygen to help her breathe.
“With this illness, I have isolated myself quite a bit because everything goes in slow motion for me,” says Thobo-Carlsen, 62.
Thobo-Carlsen wasn’t always in “slow motion.” She worked in the fast-paced travel industry for years, including for airlines, before COPD put an end to that. The disease severely damages the lung’s airways, allowing less air to be breathed in and out. An estimated 328 million people worldwide have COPD; 3 million people a year die from it, accounting for 6% of all deaths worldwide, according to the World Health Organization. While smoking is the main risk factor for COPD, up to 25% of people who develop the disease never smoked.
COPD is not curable, but it is treatable, including with the use of oxygen therapy through a nasal tube or mask. It’s not uncommon for COPD patients to need in-hospital monitoring throughout the year to make sure they are continuing to receive the proper amount of oxygen. Too much oxygen can induce headaches, sleepiness, confusion and cause damage to the lungs. Too little, and death can result in a matter of minutes.

With COVID-19 straining health care systems in the past year, hospitals in 25 countries last year turned to a new technology made by O2matic of Denmark, to help ease the burden on hospital staff. O2matic’s monitoring device and system automatically adjusts oxygen based on a patient’s condition and keeps a patient’s oxygen saturation levels in the correct range 85% of the time, compared to 47% of the time with manual oxygen treatment administered by nurses. It is also being used to help treat COVID-19 patients who need oxygen therapy.
Now O2matic has released a home version called O2matic Home Oxygen Therapy, something both patients and medical professionals welcome.
“In this time of COVID-19, especially, it is important to reduce contacts between the hospital and COPD patients,” says Dr. Thomas Jørgen Ringbæk, clinical associate professor in the Department of Clinical Medicine at the University of Copenhagen.
“Many of our very fragile patients, they are afraid of coming to the hospital for oxygen treatment, and they’re also afraid of having visits to their homes from the hospitals to check their oxygen levels,” he says.
The O2matic Home Oxygen Therapy system “allows us to keep oxygen saturated at a specified level, and we think that will provide a more optimal treatment for the patient – more time in the right range, reduced time with low oxygen saturation and reduced time with high oxygen saturation,” Ringbæk says. “Think of it as analogous to diabetes treatment, where you also want to avoid too much time with very high blood sugar and very low blood sugar.”
Thobo-Carlsen says the convenience of having the system at home would make a big difference for her. She was among the patients who tested the home unit at Hvidovre Hospital near Copenhagen.
“Sometimes I don’t need any oxygen because I’m sitting down or laying down at home,” Thobo-Carlsen says. “And other times, when I’m doing more things, I need more oxygen. With this little device, I would get more oxygen when I need it, and less when I don’t need it, which would be fantastic.”
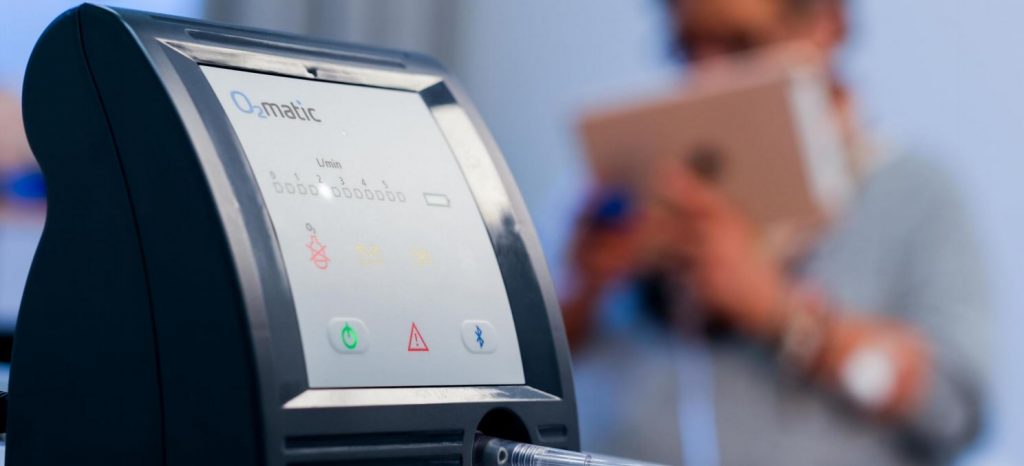
The “little device” weighs just 704 grams (about 1-1/2 pounds). Unlike its hospital sibling, the O2matic Home Oxygen Therapy unit only has one button – “on/off” – and “You really need to push it hard to turn it on or off,” says Farzad Saber, O2matic chief business development officer. “The grandchildren, for example, cannot come and visit their grandparents and start changing the configuration.”

O2matic Home Oxygen Therapy incorporates artificial intelligence. It is built on Microsoft Azure and uses Azure IoT (Internet of Things) Hub and Microsoft Intune, a cloud-based service that focuses on mobile device management and mobile application management.
The technology enables the system to automatically measure and adjust a patient’s oxygen levels, using a pulse oximeter, while sending the data to hospital staff in real time.
“We measure continuously,” Saber says. “And then our device picks up those measurements every second, and based on an algorithm, the flow of oxygen is adjusted up and down based on the patient’s need.”
That makes it easier for the staff to monitor patients and enables them to spend more time on patients in the hospital for diseases like COVID-19.
“Previously, a COPD patient had to go to the hospital to give this information to the doctor,” says Anja Rode, O2matic global product manager. “But now the patient can stay at home, and the doctor can get all the information he or she needs to adjust the treatment by using the O2matic Home Oxygen Therapy device.”

Rode, a former ICU nurse who worked in a hospital pulmonary department, cared for patients who were treated with oxygen, and saw how manually administered oxygen saturation could fluctuate for them.
“Taking this technology home to the patient and adjusting the oxygen automatically according to the patients’ needs is a huge step, and hopefully this can improve their quality of life,” she says. “With the pandemic, I also see much potential in keeping this vulnerable group of patients out of the hospitals by treating them at home, and not exposing them to a potential life-threatening virus.”
Elena Bonfiglioli, Microsoft’s managing director and regional lead for health care and life sciences in Europe, the Middle East and Africa, says O2matic’s work reflects Microsoft’s three pillars of health care: enabling better experiences, better insights and better care.
O2matic’s system “is transformative,” she says, especially because the technology itself is “almost invisible, and the experience becomes what counts.”
Saber says according to O2matic’s studies so far, automatic adjustment of oxygen levels may also help patients to be more engaged in activity.

“One of the biggest challenges for patients using oxygen therapy is that they get tired when they’re visiting people, taking their equipment, walking to friends,” he says. “When they arrive, they cannot breathe, and everybody has to wait until they get normalized again and they can start talking. It’s because they’re receiving a fixed amount of oxygen. If you are able to adjust it, they don’t get tired. In the study, if a patient receives the right amount of oxygen, they can walk longer. They can be more active. We know that we can improve the quality of life for the patients.”
It would mean a lot to Thobo-Carlsen to be able to be more physically active. When the weather is good, friends sometimes ask her to join them for a walk, but she hesitates.
“I feel like I’m slowing them down, because I have to go slow, and I don’t feel comfortable with that,” she says. There’s another reason, too, one that’s small in size but huge in importance to Thobo-Carlsen.
“I have a little granddaughter, a year-and-a-half old,” she says. “My daughter asks me if I could take care of her sometimes, and I would love to, but it’s a little bit tough.” Having the home system “would improve my quality of life quite a bit. With this, I hope that I can enjoy my granddaughter and do some more things with her than I do now.”
Lead image: Dr. Ejvind Frausing Hansen at Hvidovre Hospital in Denmark shows Lisbet Thobo-Carlsen the O2matic HOT home device. Photo courtesy of O2matic.
