Ochsner Health System: Preventing cardiac arrests with AI that predicts which patients will ‘code’
In modern hospitals, doctors and nurses are trained to rush into action when a patient “codes” – suffers a cardiac or respiratory arrest and needs immediate medical help. But what if doctors could see into the future and know who is about to code, so they could prevent a code from happening in the first place?
A new artificial intelligence tool launched by Ochsner Health System enables doctors to do just that, by analyzing thousands of data points to predict which patients will deteriorate in the near future.
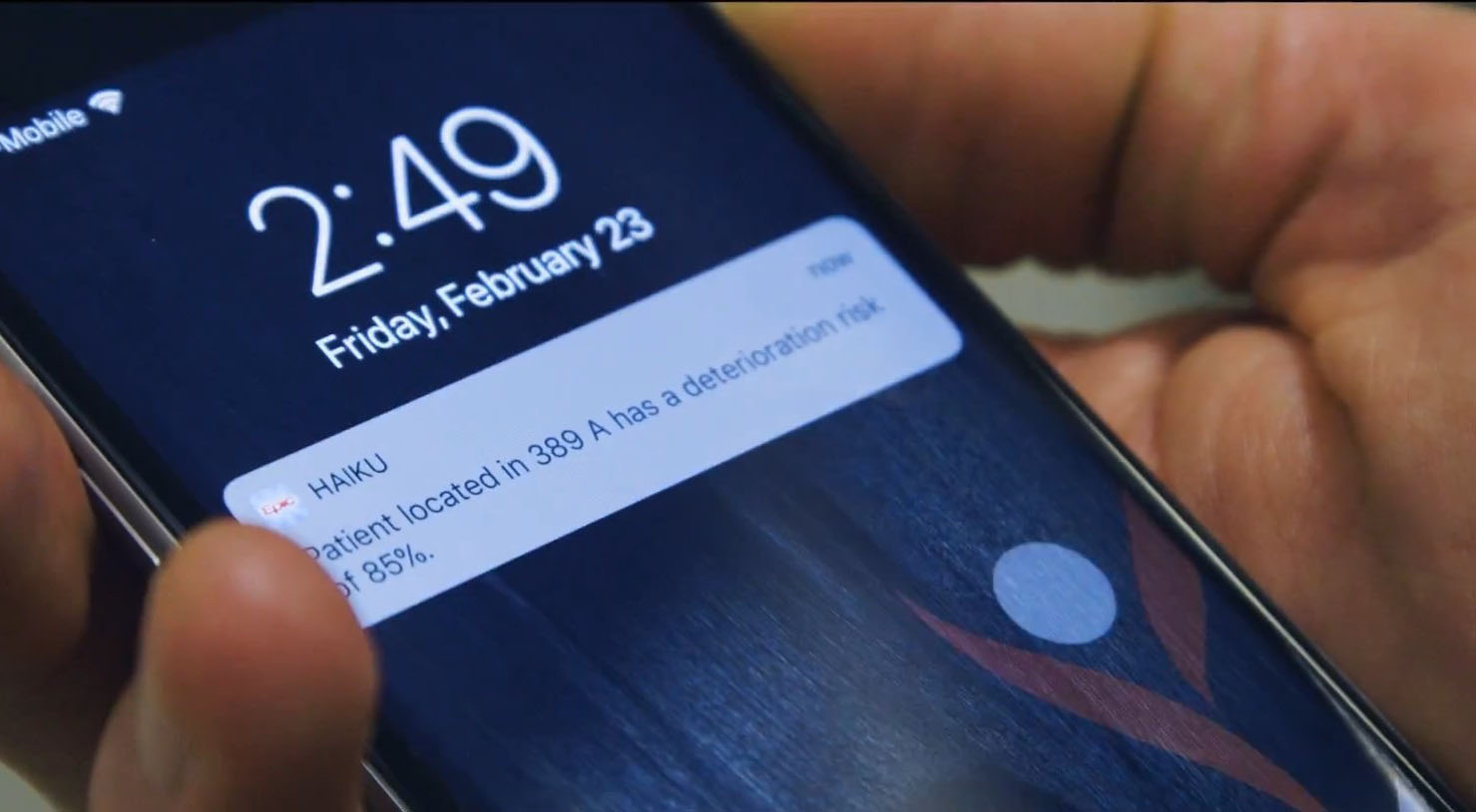
Built with a machine learning platform by health care software company Epic, the groundbreaking technology triggers “pre-code” alerts that help Ochsner’s care teams intervene sooner, treat patients more proactively and save more lives.
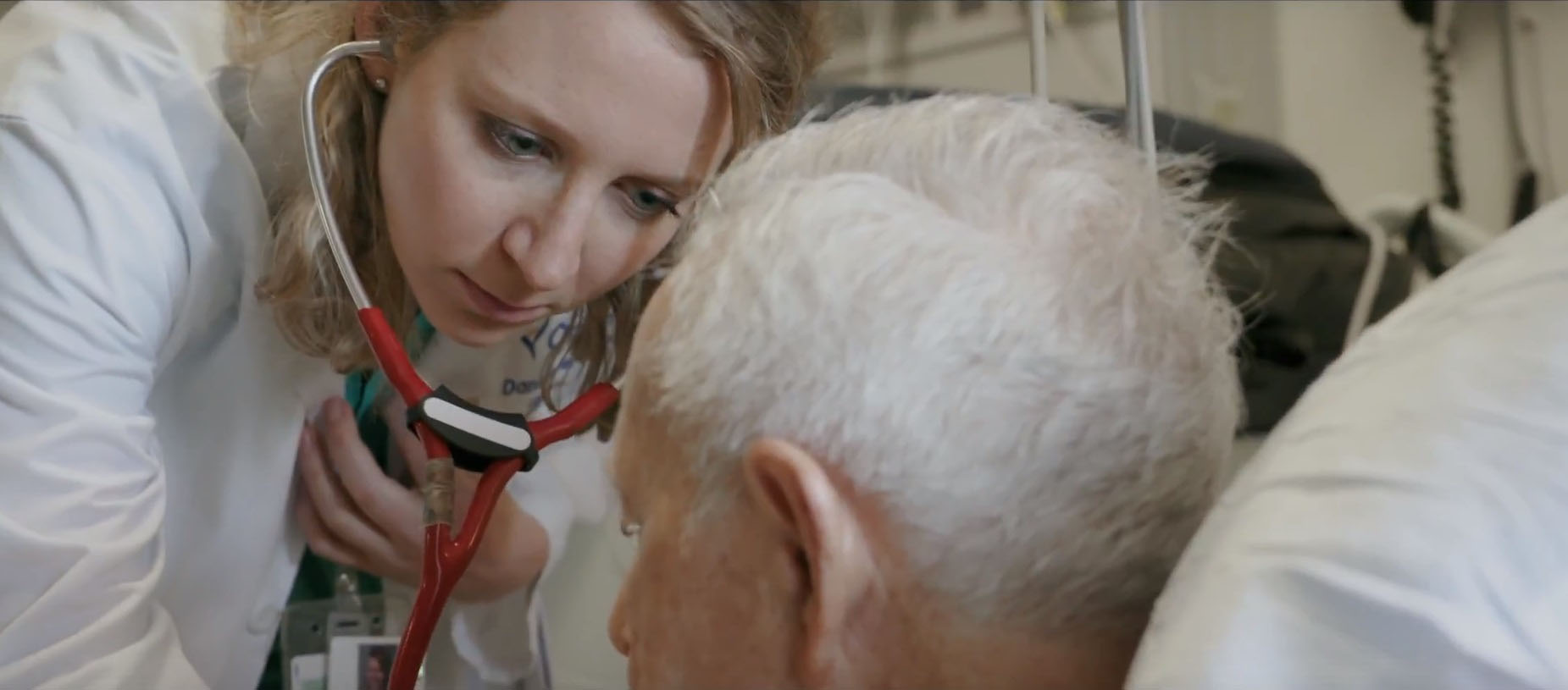
“It’s like a triage tool,” says Michael Truxillo, medical director of the rapid response and resuscitation team at Ochsner Medical Center, the organization’s flagship hospital in New Orleans.
“A physician may be supervising 16 to 20 patients on a unit and knowing who needs your attention the most is always a challenge,” he says. “The tool says, ‘Hey, based on lab values, vital signs and other data, look at this patient now.’”
In a 90-day pilot with the system last fall, Ochsner successfully reduced the hospital’s typical number of codes by 44 percent. It’s now expanding the technology to a 24-hour schedule and to more hospitals in its network, which constitutes Louisiana’s largest not-for-profit health system. Epic’s machine learning platform and model library are available to all organizations that use Epic software, regardless of whether the organizations have data scientists on staff.
Integrating AI and changing culture
The rapid rise of AI has led to many research projects for health care, but Ochsner is one of the first health systems in the country to integrate AI into patient care workflows. The foundation for its predictive tool began five years ago, when Ochsner started the task of standardizing workflows and consolidating data sources across its many hospitals.
Predictive models need massive amounts of data, and the groundwork with Epic’s comprehensive health records software now allows Ochsner to query a large database from 11 hospitals. That data enabled Ochsner to build, train and validate a model to predict patient deterioration.
“We had a vision five years ago that we knew we were going to use the data and it had to be done cleanly,” says Richard Milani, chief clinical transformation officer of Ochsner Health System and medical director of innovationOchsner, a program to revolutionize health care with new solutions.
Building the model was hard work, but integrating it into a human workflow was also tough. The technology required a new way of working. At first, some doctors thought the tool was another “scoring calculator” that identifies large groups of high-risk patients and was something a nurse could respond to.

Other times, the system triggered an alert for a patient soon after a nurse had checked vital signs and walked out of the room. Patient statuses constantly change, and the system sends only a handful of alerts a day – six to 10, out of hundreds of patients. Each alert requires attention from a provider trained in quick diagnoses and not just resuscitation.
“This is a whole different ball game that’s changing the culture,” Milani says. “We’re creating specific training that doesn’t typically exist and building teams to do this well.”
Alerts provide four-hour warning
To reduce false positives, his team trained the model for Ochsner’s population, which has a lot of patients with kidney and heart failure. Lab values worsen before a dialysis patient undergoes treatment, but the patient isn’t at risk of coding.
Similarly, LVAD patients – those implanted with a heart-assistive device – have an alarming-looking flatline for blood pressure readings, but are very much alive. Ochsner’s model accounts for both types of patients.

“Part of this project was learning what happens when you put the model in the real world,” says Jonathan Wilt, chief technology officer of innovationOchsner. “And knowing what will be hard to predict and can the model handle humans manually inputting numbers and vitals?”
The team also finetuned timing and frequency. Too few alerts missed high-risk patients, but too many produced alert fatigue. Alerts sent too soon didn’t convey urgency, while those sent too late didn’t allow for interventions.
A four-hour warning turned out to be ideal, giving enough time for a rapid response provider to finish what she’s doing, walk – not run – to a patient’s room and conduct an evaluation. Interventions may be a medication change, transfer to ICU or another form of elevated care.
“The model is strong, but we wanted to know, ‘With the information, can you do something to change what would have been the course of history?’” Milani says.
A trained data scientist, Wilt is also using Epic’s advanced machine learning tools to predict pressure ulcers and hospital-acquired infections. But Epic’s platform enables health systems of all sizes – including those without AI experts – to quickly build and integrate models.
The company’s library of machine learning models and a growing “algorithm economy” among organizations that use Epic software also help health systems, whether they want to predict sepsis, readmission risk or staffing levels.
“This means you don’t have to have data scientists in your organization to take advantage of machine learning,” says Seth Hain, Epic’s director of analytics and machine learning.
Powered by Microsoft Azure, the platform is largely invisible to end users, so all they see is key, real-time information – an alert, recommended action or dashboard analytics. “It gives the provider more time to focus on the patient,” Hain says.
Truxillo says Ochsner’s providers have come to embrace the predictive tool.
“Clinicians are inherently skeptical,” he says. “They’re wondering, ‘Is artificial intelligence going to replace doctors?’”
The answer is no; doctors still must diagnose patients, he says. The tool helps them prioritize care and synthesize the constant streams of changing information that doctors must track.
“This technology definitely helps save lives,” Truxillo says. “If we can make a difference for patients because of the alerts, we’ve done a tremendous service to them, their families and the community.”
Learn how health organizations across the globe are partnering with Microsoft.
Top image: Michael Truxillo, medical director of the rapid response and resuscitation team at Ochsner Medical Center. Photo courtesy of Ochsner Medical Center.








