
Remote Australian community harnesses mixed reality and space technologies to deliver better healthcare
Dargo is a remote town in far East Gippsland, Victoria, Australia, nestled in the foothills of the Victorian Alps. The town is home to a tight-knit community of around 100 people – some of whom have lived in Dargo all their lives.
“You know everybody and everyone knows you, so there are always friends around, and the community connections are really strong,” says Sue Neale, a Nurse Administrator at Dargo Bush Nursing Centre who has lived in the town for 10 years.

“The population in Dargo is very diverse. We have people aged from babies right up to their eighties. We have single people and elderly people who are quite colourful characters, and we’re seeing more families moving to the area with children as well. Everyone has a lot of energy in this town.”
The Dargo Bush Nursing Centre plays a vital role in helping the remote community access healthcare services. The centre is staffed by a small number of senior nurses, such as Sarah Carr, who provide acute care to patients and focus on their emotional and social wellbeing.
“We are here for anyone in the community who might have any health issues, from pregnancy [and] even conception issues all the way through to palliative care, funeral arrangements, bereavement counselling and anything in between,” Carr says.
Longtime resident Phil Davies, a committee member of Dargo Bush Nursing Centre, describes it as “the lifeline of the community”.
“The centre is so important,” he says. “I recently suffered a heart attack and didn’t know what was happening – I thought it was indigestion – but the bush nurses here in Dargo saved my life. They took care of me at the centre while I waited for an ambulance.”

Remote healthcare roadblocks spur desire for telemedicine
Dargo Bush Nursing Centre is one of 15 bush nursing centres in Victoria and one of six in the East Gippsland region. It works in partnership with Bairnsdale Regional Health Service (BRHS).
Sometimes patients present to bush nursing centres with conditions that nurses can’t treat independently, and for which they need specialist advice. However, travelling to see a specialist can cost patients time away from work and properties, as well as large sums for fuel and accommodation.
“The time and the travel that it takes to actually get to a medical professional if you are earning a living on the farm … that’s pretty much a whole day out that you have to travel to see someone for your care,” says Carr. Some Dargo residents have been forced to delay specialist appointments because of the impact on their livelihood.
Small staff numbers also make it challenging for bush nursing centres to treat patients, particularly during holiday periods when town populations grow significantly.

According to Julie Lawrence, Sub-Regional Partnerships and Innovation Lead at BRHS, “These small bush nursing centres that might have five visits a day can have up to 50 when there are visitors camping and hiking.”
These challenges spurred a desire for telemedicine in remote communities across the East Gippsland region. However, a lack of fast and reliable cloud connectivity in many of the communities, including Dargo, prevented BRHS from rolling out telemedicine sooner.
Boosting the bandwidth in space
Microsoft launched Azure Space two years ago and since then have been working to democratise access to Space through key industry partnerships and new product releases. Teaming up with Microsoft partner Velrada, BRHS wanted to pilot a first-of-its-kind telemedicine solution in Dargo that used mixed reality technology. But the town’s limited connectivity made this impossible.
“The infrastructure wasn’t there to support the community,” says Darin Roy, East Gippsland Telehealth Project Lead at BRHS. “There just wasn’t the capacity to have the clear videoconference conversations you needed for it to work.”
With the help of Davies, an electrician by trade, BRHS installed a SpaceX Starlink satellite dish at the Dargo nursing centre to ensure fast and reliable connectivity to the cloud. It increased the centre’s download speeds from as little as 3 megabits per second to 290 megabits per second.
“Basically, all I had to do was screw the satellite dish to the roof, plug it in and it found the satellite [in space] straight away,” Davies explains. “As an electrician, I thought, ‘Wow, how easy is this?’
It’s incredible to think that space is making a difference to the health of our community.
Mastering mixed reality to overcome geographical barriers
Once the satellite link was in place at the Dargo centre, BRHS conducted an eight-week pilot of the telemedicine technology using Velrada’s Mixed Reality as a Service (MRaaS). It helped specialists and general practitioners (GPs) outside the town treat patients remotely using Microsoft’s mixed reality technologies and Azure Space cloud infrastructure.

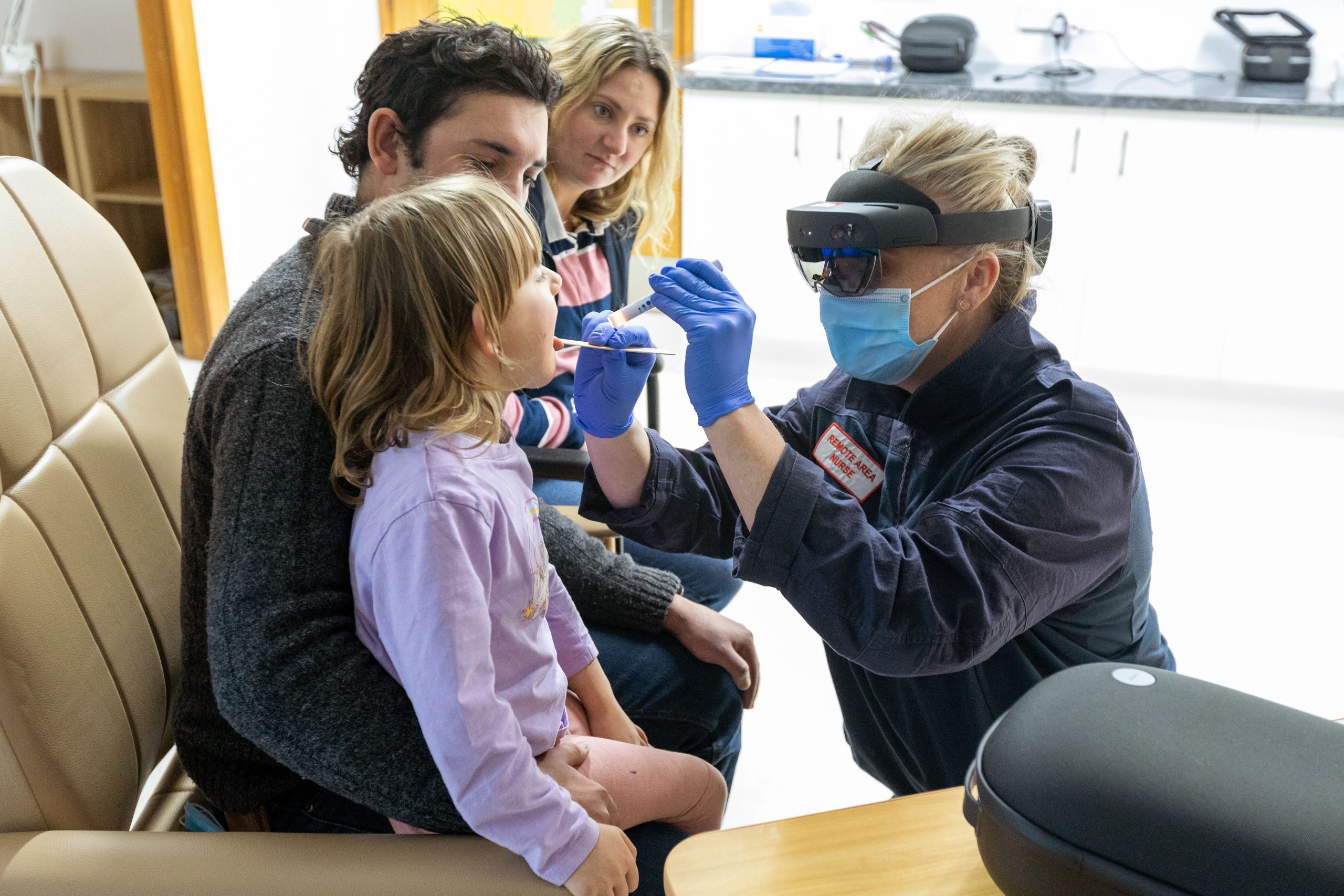
Wearing a Microsoft HoloLens headset, nurses could facilitate appointments in Microsoft Teams.
The Mixed Reality solution uses Dynamics 365 Remote Assist to connect the wearer to a Teams call. It allows the specialist to be able to see what the nurse can see and to ‘draw’ on the patient, share imaging, and go through checklists as they need. It connects the Specialist with the nurse in such a way that the experience for the patient is much like having the specialist physically there.
“The HoloLens device is a game changer [for] our telehealth,” says Carr. “You can get right up close to the area that needs reviewing and the doctor will see exactly what we’re seeing.”
Patients can hear what the specialist or GP is saying through a speaker connected to the headset. The mixed reality environment also enables nurses and physicians to draw and annotate on the holographic screen for further instructions.
“It allows the nurses to be hands-free and to communicate with the physician more easily,” says Neale. “And the patients can explain what’s wrong with them a lot more clearly and be supported with the nurses.”
Dr Chris Sia, a nephrologist at Alfred Hospital in Melbourne, participated in the pilot and had “a really positive” first experience using the telemedicine solution.
“What I found most impressive was the mobility that it provided, and I really felt like the nurse was my eyes and I was in the room,” he explains.
“In my field of nephrology, sometimes it’s really important to get a good look at the patient’s legs, because if they’re carrying too much fluid, that’s often where the fluid can accumulate.”

Sia believes the mixed reality environment also fosters better engagement from patients and enables nurses to play a more active role in providing treatment.
Successful pilot prompts regional roll-out
Twelve telemedicine appointments were conducted in Dargo during the eight-week pilot. According to Roy, half of them involved specialists located four-and-a-half hours’ drive away in Melbourne.
In one instance, the mixed reality solution enabled an orthopaedic surgeon to view the location and characteristics of bruises and inflammation on a patient, Roy says.
“[In another case,] there was a 14-month-old child who avoided a long trip to hospital after suffering envenomation from a bite,” he says. “We were able to connect them with a paediatrician who treated the child remotely through the HoloLens. The child’s parents were very happy and comfortable with the experience.”
Farmer Emily Theodorou was another Dargo resident who saved a significant amount of time and money thanks to the town’s new telemedicine facility.
“My daughter had to have her tonsils out, so that was a trip to Melbourne,” she explains. “We needed to have a follow-up appointment six weeks later with the surgeon. For my family to go and see a medical specialist in Melbourne, we are looking financially at an outlay of at least $800 to $1,000 once we factor in fuel, accommodation and just time in general.
However, we didn’t have to go for the follow-up appointment because we were able to use [telemedicine] in the Dargo Bush Nursing Centre. The surgeon was actually able to see down where he needed to see as if he was looking at it.



Following the success of the trial, BRHS shifted from renting Velrada’s MRaaS platform to owning and managing technology itself. The team plans to equip five other bush nursing centres – Buchan, Cann River, Ensay, Gelantipy and Swifts Creek – with HoloLens units. Dargo and Cann River will upgrade their satellite connectivity so they can adopt the telemedicine model. BHRS will also use HoloLens devices at Omeo District Health and Orbost Regional Health services, Gippsland Lakes Complete Health community health agency and Maddocks Gardens residential aged care facility.
“The learnings we’ve had from Dargo, even though it was quite a small and short pilot, has set us up for success across the region,” says Lawrence. “It means that our whole area will be connected, and that’s quite exciting.”
BRHS Chief Executive Robyn Hayles says the organisation is proud to be a pioneer of virtual medical technology.

“The telemedicine solution is absolutely groundbreaking for healthcare in East Gippsland,” she says. “By bridging the geographical gap between patients and specialists, we can better meet the medical needs of our diverse population while minimising disruption to their lives and livelihoods. The combination of space satellite and mixed reality technologies have taken our service to the next level of care.”
As for Dargo residents like Davies, they no longer have to worry about moving closer to a hospital to receive the treatment and care they need.
“I always said I would never leave Dargo unless I was in a box,” he says. “That box is now further away.”










