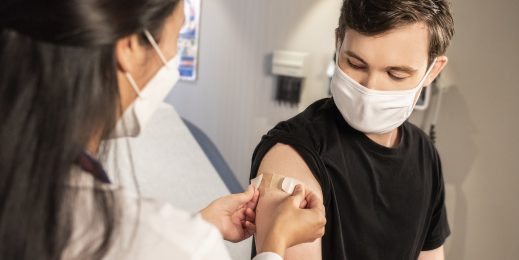
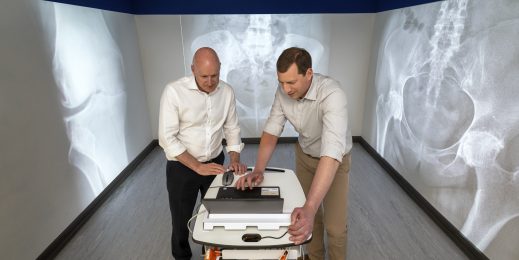
Health
No one likes waiting on the phone for a GP appointment. So why do we still do it?
Patient Access is giving people more control over their healthcare
When you need to see your GP, do you pick up your phone and tap on the “call” icon or the “web browser”?
In today’s fast-paced world, it’s odd that a national patient survey conducted by the NHS last year found 79% of us like to ring up a receptionist to book an appointment for us – and suffer the inevitable queue and hold music – rather than logging on to a website or app and doing it ourselves (10%).
One reason for this could be that a lot of GP surgeries in England don’t have a website that lets patients book appointments. Another is that some websites, when they do exist, are clunky and hard to use. Yet another could be that older people tend to see doctors more often and they might be more comfortable using a phone to speak to someone.
These reasons (and many more) are surely factors, and they are all contributing to the same problem – local NHS services are not embracing technology fast enough.
Patient Access is aiming to change that. It’s a website that lets people book GP appointments, order prescriptions, view their medical record and message their GP surgery using whatever device they want, wherever they are. A new feature called Proxy Access lets you complete all these tasks on behalf of someone else, such as an elderly relative.
The team behind the services are experts at healthcare, as they also run Patient.Info, one of the most popular medical websites in the UK. More than 100 million people logged on to the site in 2018 to read articles about healthcare, check symptoms and learn to live a healthier life, and more than 60% of GPs in England have access to it.
They also produce a newsletter that’s sent to 750,000 subscribers and around 2,000 leaflets on health conditions and 850 on medicines.
People can access Patient.Info 24 hours a day, seven days a week. It’s the same for Patient Access but web traffic spikes every morning when people want to book appointments to see their GP. To handle that demand, Patient Access runs on Microsoft’s Azure cloud platform. As well as being reliable and stable, all patient data is protected by a high level of security – Microsoft employs more than 3,500 dedicated cybersecurity professionals to help protect, detect and respond to threats, while segregated networks and integrated security controls add to the peace of mind.
“About 62% of GP practices use Patient Access,” says Sarah Jarvis MBE, the Clinical Director behind the service. “They’re using it to manage their services, manage appointments, take in repeat medications, consolidate a patient’s personal health record and even conduct video consultations.
“Just imagine your GP being able to conduct video consultations. If you’re aged 20 to 39 you might not want or need to have a relationship with a GP because you don’t need that continuity of care.
“But imagine you are elderly and housebound, and a district nurse visits you. They phone your GP and say: ‘Could you come and visit this patient’, but the GP is snowed under and can’t get there for a couple of hours. The district nurse is also very busy and must visit someone else.
“Now, with Patient Access, a Duty Doctor can look at someone’s medical record and do a video consultation in five minutes. If the patient needs to be referred, the GP can do it there and then from inside the system. The possibilities are endless, and older people, especially, have so much to gain from this.”
Elderly people or those with limited mobility can often struggle to get to GP surgeries, so video consultations can be a perfect alternative.
The latest figures from NHS Digital reveal that there were 307.2 million appointments with a GP or GP surgery staff (osteopath, counsellor, physiotherapist, nurse etc) in England between June 1, 2018, and May 31, 2019 – around 233.8 million of those were face-to-face, while just 1.3 million were via a video link or online. Just under 90% of appointments in GP surgeries were attended but this rate rises to 93.5% for telephone appointments. The NHS doesn’t break out attendance figures for online and video link appointments but it would be reasonable to expect they are high, as people can use their own devices to log on from home.
Patient Access can also help those who can’t (or won’t) take time off work to see their GP. A recent study by health and wellbeing provider Benenden Health found that a third of the 2,000 Brits polled felt guilty about taking time off work to see a doctor, and only half said their manager was flexible when they needed to book an appointment. Shockingly, a fifth have had to wait until their shift at work finished before they could go to A&E.
“We know that people do pretty much everything online,” adds Jarvis, who is also a GP, GP trainer and resident doctor for the Jeremy Vine show on BBC Radio 2. “We know that more than 85% of the population have access to a smartphone, and an even greater proportion has access to the internet. We also know that people these days are not prepared to access healthcare services solely between the hours of 9am and 5pm. However, as people live longer, they will have developed more complex medical conditions.
“Patient Access puts people in control of their healthcare. They can access their medical records and share them securely with healthcare professionals; order and manage prescriptions and determine which pharmacy they are sent to; message their GP and book face-to-face, video and phone appointments.”
By giving people the tools available in Patient.Info and Patient Access, Jarvis hopes that people will “understand their symptoms before they have a professional diagnosis, to work out whether they need emergency care, to see a GP or treat themselves”.
It all helps to ease the burden on the NHS, which the British Medical Association has warned is at breaking point. There are around 34,000 GPs in the UK, but a report by the King’s Fund, Nuffield Trust and Health Foundation in March stated that the shortfall in the number of GPs is so serious that it “cannot be filled at all”. Meanwhile, demand is rising, with the number of GPs per 100,000 people falling from nearly 65 in 2014 to 60 last year. The average doctor now has 125 more patients to look after than they did in 2014.
The health sector is increasingly turning to technology to help ease the burden. In June, the Welsh government gave all NHS staff in the country access to Microsoft 365, including Teams and Outlook, to help them communicate, collaborate and securely share patient information. The move is also expected to help NHS staff save money and time by not having to travel to face-to-face meetings, freeing them up to focus on patients who need the most help.
NHS Scotland is merging more than 100 separate computer systems and will give its 161,000 staff access to Office 365 so they can spend more time focusing on patients.
It is all underpinned by the cloud. In January 2018, Jeremy Hunt, then Secretary of State for Health and Social Care, signed off on guidance that helped public health organisations move data from on-site servers to cloud services in data centres run by companies such as Microsoft.
In one stroke, the NHS can now explore cheaper and more flexible technology-based solutions that can help them serve people across England in a way that suits them.
Jarvis adds: “We live in a country of contrasts. The older you are, the less technologically adept you are likely to be. However, the older you are, the more likely you are to need easy access to online healthcare services. I’ve become aware of how much I use technology on a day to day basis. So, I knew we had to have an amazing user experience that would be easy to use.”
Jason Keane, Chief Executive of Patient Access and Patient.Info, says the company spoke to many people to understand what they wanted.
“We talked to patient groups, surveyed more than 500,000 people in the UK and worked with about 50 GPs to understand what they need,” he says. “We wanted to find out how we can make all their lives easier. What features will take some of the pressure off GP practices? What do users want to see? The results spoke for themselves.”
What people wanted was not only easy access to healthcare services via the internet, but a simple system that let family members and carers make decisions on their behalf.
Keane and Jarvis rolled out Proxy Access, allowing people to book appointments, order prescriptions and message GP surgeries for someone else. It has received more than 1.5 million prescription requests since its launch.

Jarvis adds: “Patient Access can help if you’re looking after an elderly relative and need to order a repeat prescription for them, book an appointment on behalf of your six-year-old son or daughter, or you’re one of many people across the country who are regularly caring for young and old people. They need as much help as possible, and we can make their life slightly easier while ensuring safeguards are in place for confidentiality and security.”
The aim is to help individuals manage their healthcare, and that will spread to communities, regions and, eventually, the entire country.
Last year, the Government announced a £20.5bn increase in NHS funding every year by 2023 in a move the then Secretary of State for Health and Social Care, Jeremy Hunt, said would help the National Health Service “write an entirely new chapter in its history”. To ensure patients in England remain the heroes of that book, the NHS needs people to take more control of their health and how and when they receive care.
Patient Access is helping the NHS write a bright, new future.