Skip the hold music and meet Premera Scout, a chatbot that helps you with health care
When dealing with health care, sometimes you don’t want to wade through a web site or app, and you really don’t want to make a call and hear, “Please continue to hold.” You just want to type a question and get an answer.
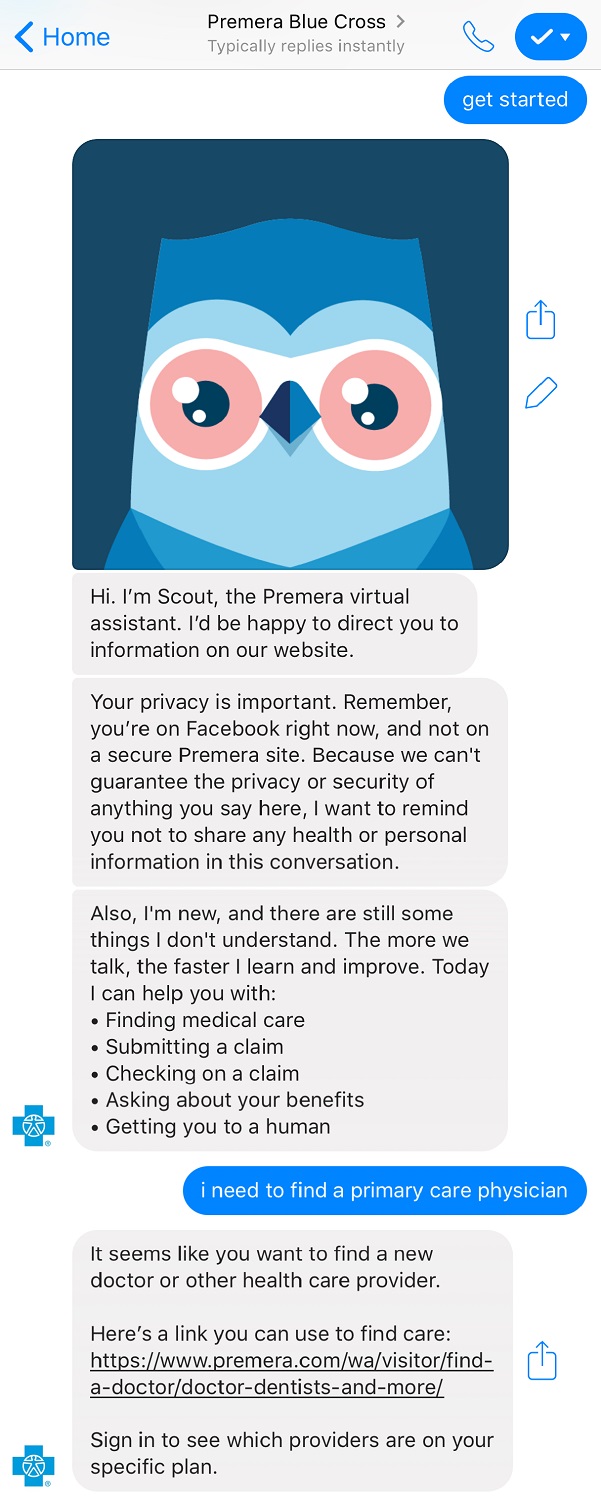
To the rescue: Premera Scout, a new chatbot created by Premera Blue Cross, the largest health plan in the Pacific Northwest. Launched in July on Facebook Messenger, the virtual assistant uses easy-to-understand, text-based chat to help customers quickly know where to get information on claims, benefits and other Premera services. The Facebook Messenger version of Premera Scout is built with frequently asked questions in mind, but is not intended to give or receive customer-specific health information.
“Health care can be very complicated and we’re trying to make it simpler,” says Neil Lazo, director of products, mobile at Premera, which is based near Seattle in Mountlake Terrace, Washington.

“Premera Scout is the platform where you can talk to us in a natural way and we’ll get you the answer in a way you actually speak, and not how health insurance people speak.”
The chatbot is part of a growing trend of intelligent virtual assistants enriching human customer service, fueled by advances in artificial intelligence (AI) and the boom in messaging apps. The work stems from Premera’s digital and innovation teams and the Microsoft Healthcare initiative, both transforming health care with AI, cloud and other modern tools.
“Health care has been kind of slow at adopting new technology,” says Torben Nielsen, Premera’s vice president of innovation and strategic investments, who runs the Premera Test Kitchen, the health plan’s innovation team. “I have a saying: ‘I work in health care during the day and go home at night to the 21st century.’”
From old-fashioned fax machines to clunky systems for finding doctors, the industry is often tough for consumers to navigate, he says. His team of developers, designers and experts are working with Microsoft and startups on technology that can guide consumers, streamline scheduling and predict health issues. And it recognizes that many people would rather chat than call a maze of phone options and listen to hold music.
“At Premera, we’re looking at the consumer experience and want to make it as seamless and frictionless as possible,” Nielsen says.
With an avatar of a serene blue owl, Premera Scout helps customers “self-serve” basic questions at any hour, while giving customer-service employees more time to handle complicated requests.
“Sometimes people are more reserved talking to a person, but feel like they have more freedom to ask any question with a robot,” says Lazo. He says Premera Scout doesn’t replace the “world-class support” of Premera’s customer-service representatives, but gives members another avenue to communicate.
“It understands you as a human being and can have a conversation with you in an easy way,” Lazo says.
To build Premera Scout, the health plan used the Microsoft Health Bot service, an AI solution created for the health industry. Built on Azure to meet stringent health-privacy laws, the tools integrate medical content and triage protocols with Azure Cognitive Services, including Language Understanding for natural language processing and Text Analytics for understanding emotional sentiment.
The out-of-the-box solution includes an extensible platform, built-in compliance constructs and “Healthcare AI,” a set of systems that comprise complex medical vocabulary, symptom checker protocols and language models for health care terminology.
“The Health Bot service empowers health care organizations to build intelligent and compliant virtual health assistants and chatbots that improve processes, outcomes and self-service options, and reduce costs,” says Hadas Bitran, head of Microsoft Healthcare Israel, which developed the service.
The solution powered Premera’s ability to build a bot that can understand how members talk, detect frustration and respond helpfully.

“People don’t talk in the same way. They use slang, say ‘yes’ in different ways or spell ‘anesthesiology’ wrong,” says Lazo. “On top of that, many people have a hard time with health insurance, because they’re asking questions during a time of need and sometimes they’re angry.”
In the future, the health plan will build new scenarios for Premera Scout based on continuously incoming data from customer chats and calls. It will embed the bot in its web site, mobile apps and other messaging channels for wide availability. And it will create a secure route for accessing individual account information.
As Premera Scout matures, the work won’t just benefit the health plan’s 2 million customers in Washington and Alaska. It will help improve the Microsoft Health Bot service, which is currently in private preview with Premera and two other health partners. General availability is expected in 2019.
“Premera’s commitment to innovation and collaboration has helped make this partnership very successful,” says Bitran. The collaboration has also been productive for Premera.
“We have a lot of the insights from a health care perspective and Microsoft obviously knows AI and technology,” says Nielsen. “It’s been a beautiful partnership.”
All photos courtesy of Premera Blue Cross.









